(20-RES) Cavernous Transformation of the Portal Vein in the Setting of Protein C Deficiency
Thursday, October 9, 2025

Abigail Carroll, DO
Internal Medicine
Oklahoma State University Medical Center
Owasso, Oklahoma, United States
Presenter(s)
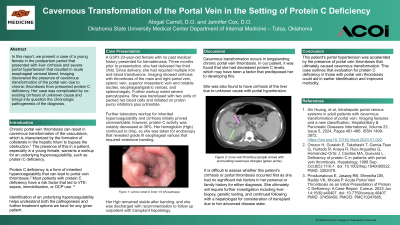
Clinical Scenario or Case: A G3P3 23-year-old female with no past medical history presented to the emergency department (ED) for hematemesis. Three months prior to presentation, she had delivered her third child. Since delivery, she had required multiple iron and blood transfusions. In the ED, laboratory evaluation revealed severe pancytopenia. Computed tomography (CT) of the abdomen and pelvis showed cirrhosis with thrombosis of the main and right portal vein, splenic vein, superior mesenteric vein and notable ascites, esophageal/gastric varices, and splenomegaly. She was transfused with two units of packed red blood cells and initiated on proton pump inhibitors plus octretide.
Further laboratory workup for inherited hypercoagulability and cirrhosis initially proved unremarkable; however, protein C activity was notably decreased at 36%. Her hemoglobin (Hgb) continued to drop, so she was taken for endoscopy that revealed grade III esophageal varices that required extensive banding. Her Hgb remained stable and she was discharged with recommendation to follow up outpatient with transplant hepatology.
Evidence/Literature Review: Chronic portal vein thrombosis can result in cavernous transformation of the vasculature, which is characterized by the formation of collaterals in the hepatic hilum to bypass the obstruction. The presence of this in a patient, especially in a young female, warrants a workup for an underlying hypercoagulability, such as protein C deficiency.
Unique Aspects of Case: This case highlights a young postpartum female that presented with a variceal bleed and was found to have decompensated liver cirrhosis and severe portal hypertension from cavernous transformation of the portal vein. The etiology of her case is puzzling and warrants into question the chronologic pathogenesis of her disease.
Recommendations/Conclusions: This patient's portal hypertension was accelerated by the presence of portal vein thrombosis that ultimately caused cavernous transformation. This case outlines that evaluation for protein C deficiency in those with portal vein thrombosis could aid in earlier identification and improved morbidity.
Further laboratory workup for inherited hypercoagulability and cirrhosis initially proved unremarkable; however, protein C activity was notably decreased at 36%. Her hemoglobin (Hgb) continued to drop, so she was taken for endoscopy that revealed grade III esophageal varices that required extensive banding. Her Hgb remained stable and she was discharged with recommendation to follow up outpatient with transplant hepatology.
Evidence/Literature Review: Chronic portal vein thrombosis can result in cavernous transformation of the vasculature, which is characterized by the formation of collaterals in the hepatic hilum to bypass the obstruction. The presence of this in a patient, especially in a young female, warrants a workup for an underlying hypercoagulability, such as protein C deficiency.
Unique Aspects of Case: This case highlights a young postpartum female that presented with a variceal bleed and was found to have decompensated liver cirrhosis and severe portal hypertension from cavernous transformation of the portal vein. The etiology of her case is puzzling and warrants into question the chronologic pathogenesis of her disease.
Recommendations/Conclusions: This patient's portal hypertension was accelerated by the presence of portal vein thrombosis that ultimately caused cavernous transformation. This case outlines that evaluation for protein C deficiency in those with portal vein thrombosis could aid in earlier identification and improved morbidity.
