(69-RES) A Case of Mistaken Identity: Differentiating Pulmonary Hypertension Subtypes in a Complex Presentation
Thursday, October 9, 2025

Megan Rochford, DO
Internal Medicine
Kettering Health Dayton
Dayton, Ohio, United States
Presenter(s)
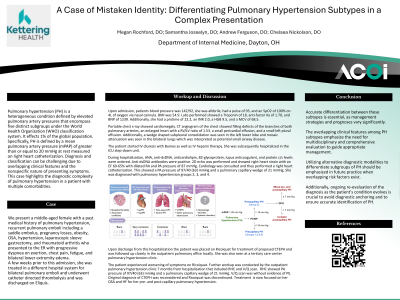
Clinical Scenario or Case: We present a middle-aged female with progressive dyspnea on exertion, fatigue, and lower extremity edema. The patient had a history of pulmonary hypertension, recurrent pulmonary emboli including a saddle embolus, pregnancy losses, obesity, OSA, hypertension, laparoscopic sleeve gastrectomy, and rheumatoid arthritis. Upon initial workup, CTA was significant for bilateral pulmonary emboli with possible left lower lobe infarct and evidence of right heart strain. Subsequent RHC was suggestive of CTEPH and the patient was placed on Ricoiquat for treatment; however, the patient experienced worsening of symptoms. On further workup, repeat RHC and V/Q scan showed evidence to suggest a combination of pre- and post-capillary pulmonary hypertension in place of her initial diagnosis of CTEPH. Riociquat was discontinued with further treatment focused on her OSA and HF.
Evidence/Literature Review: As pulmonary hypertension has been a primary focus of many research studies, accurate classification continues to play a role in treatment guidelines. However, this remains a challenge, as numerous cases of PH have been initially misdiagnosed as CTEPH. Additionally, recent literature has proposed modalities for establishing an accurate diagnosis of CTEPH utilizing specific parameters on echocardiography.
Unique Aspects of Case: This case highlights the diagnostic complexity of pulmonary hypertension WHO classifications when features of multiple subgroups are present simultaneously. This patient’s medical history of numerous thrombotic events in the setting of untreated comorbid conditions, complicated her initial diagnosis and therefore treatment.
Recommendations/Conclusions: The overlapping clinical features among PH subtypes emphasize the need for multidisciplinary and comprehensive evaluation to guide appropriate management. Utilizing alternative diagnostic modalities to differentiate subgroups of PH should be emphasized in future practice when overlapping risk factors exist. Additionally, ongoing re evaluation of the diagnosis as the patient’s condition evolves is crucial to avoid diagnostic anchoring and to ensure accurate identification of PH.
Evidence/Literature Review: As pulmonary hypertension has been a primary focus of many research studies, accurate classification continues to play a role in treatment guidelines. However, this remains a challenge, as numerous cases of PH have been initially misdiagnosed as CTEPH. Additionally, recent literature has proposed modalities for establishing an accurate diagnosis of CTEPH utilizing specific parameters on echocardiography.
Unique Aspects of Case: This case highlights the diagnostic complexity of pulmonary hypertension WHO classifications when features of multiple subgroups are present simultaneously. This patient’s medical history of numerous thrombotic events in the setting of untreated comorbid conditions, complicated her initial diagnosis and therefore treatment.
Recommendations/Conclusions: The overlapping clinical features among PH subtypes emphasize the need for multidisciplinary and comprehensive evaluation to guide appropriate management. Utilizing alternative diagnostic modalities to differentiate subgroups of PH should be emphasized in future practice when overlapping risk factors exist. Additionally, ongoing re evaluation of the diagnosis as the patient’s condition evolves is crucial to avoid diagnostic anchoring and to ensure accurate identification of PH.
