(3) Telemetry monitoring, a process improvement project to improve appropriate use

Stephanie Clauss, DO
IM
University of Miami
Cooper City, Florida, United States
Presenter(s)
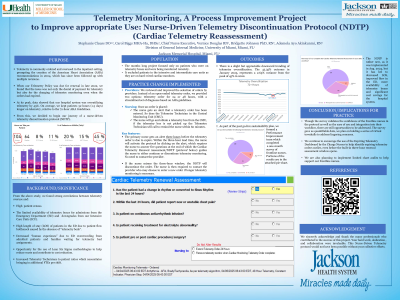
Background: Telemetry is commonly ordered and overused in the inpatient setting. When the Telemetry Policy was due for renewal in late 2022 in our hospital system, we found that the issue was not denial of payment for telemetry but overcharging for telemetry that might not have been provided due to breaks in the continuity of coverage.
Methods: The study focused only on patients who were on telemetry boxes and being remotely monitored. High telemetry utilization was found to cause a high length of stay (LOS) and patient flow concerns necessitating the need for a change. On average, we kept patients 32 hours (1.3 days) longer on telemetry relative to the 72-hour AHA Guidelines. From this we decided to begin the journey of a nurse driven telemetry protocol. The first step was improving the selection of the order for physicians. Once an order is placed, the nurse gets an alert that a telemetry order has been entered, so does the Telemetry Technician in the Central Monitoring Unit (CMU). A key feature of the Nurse-Driven Telemetry Protocol (NDTP) is that the primary nurse gets an alert three hours before the order is due to expire. Within the three-hour lead time, the nurse will activate the NDTP by clicking on the alert, then answer five questions within the three-hour window. If the nurse answers yes to any of the questions the telemetry order automatically renews for 24 hours.
Results: This protocol is rather new and was implemented in August of 2024 but has led to decreased length of stay as well as more availability of telemetry boxes and cost savings for the hospital system.
Conclusions: In conclusion going forward we hope to continue to reduce length of stay and continue to improve the appropriate use of telemetry.
Methods: The study focused only on patients who were on telemetry boxes and being remotely monitored. High telemetry utilization was found to cause a high length of stay (LOS) and patient flow concerns necessitating the need for a change. On average, we kept patients 32 hours (1.3 days) longer on telemetry relative to the 72-hour AHA Guidelines. From this we decided to begin the journey of a nurse driven telemetry protocol. The first step was improving the selection of the order for physicians. Once an order is placed, the nurse gets an alert that a telemetry order has been entered, so does the Telemetry Technician in the Central Monitoring Unit (CMU). A key feature of the Nurse-Driven Telemetry Protocol (NDTP) is that the primary nurse gets an alert three hours before the order is due to expire. Within the three-hour lead time, the nurse will activate the NDTP by clicking on the alert, then answer five questions within the three-hour window. If the nurse answers yes to any of the questions the telemetry order automatically renews for 24 hours.
Results: This protocol is rather new and was implemented in August of 2024 but has led to decreased length of stay as well as more availability of telemetry boxes and cost savings for the hospital system.
Conclusions: In conclusion going forward we hope to continue to reduce length of stay and continue to improve the appropriate use of telemetry.
