(62-STU) Impact of Socioeconomic and Demographic Factors on In-Hospital Mortality in Sepsis: Insights from the 2020 NIS
Friday, October 10, 2025

Harman Gill, n/a
Medical Student
Future Forwards Research Institute
Fair Lawn, New Jersey, United States
Presenter(s)
Introduction/Background: Sepsis is a life threatening condition that occurs when an infection disseminates throughout the body and causes a widespread inflammatory response. This study aims to explore the different socioeconomic variables and risk factors that may impact patients' outcomes when diagnosed with sepsis.
Methods: We performed a national retrospective analysis using the 2020 NIS database that included 596,093 patients diagnosed with sepsis. Bivariate χ² and log-total-charges regression tests were run to identify differences in outcomes and mortality by sex. Survey-weighted logistic regression analysis was run to identify rates of in-hospital mortality. Linear regression was used to identify trends in length-of-stay.
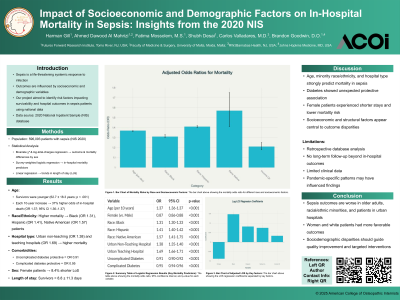
Results/Discussion: Survivors were younger (mean 62.7 ± 18.3 y; p < .001) and had shorter stays (8.8 ± 11.3d). Every 10-year increase in age increased odds of in-hospital death by 37% (OR 1.37; 95% CI 1.36–1.37). Black (OR 1.31; 1.30–1.33), Hispanic (OR 1.41; 1.40–1.42), and Native Americans (OR 1.57; 1.41–1.75) patients faced higher mortality. Treatment in urban non-teaching (OR 1.38; 1.35–1.40) and urban teaching hospitals (OR 1.69; 1.66–1.71) conferred higher mortality. Uncomplicated (OR 0.91; 0.90–0.92) and complicated diabetes (OR 0.95; 0.94–0.96) were associated with slightly lower odds of mortality. Female sex shortened stays by 8.4%.
Conclusions: Our results indicated that patients with sepsis from poorer sociodemographic areas, minorities, and the elderly had an increase in unfavorable outcomes, and longer lengths of stay. Conversely females and white patients were shown to have shorter LoS and lower rates of mortality.
Methods: We performed a national retrospective analysis using the 2020 NIS database that included 596,093 patients diagnosed with sepsis. Bivariate χ² and log-total-charges regression tests were run to identify differences in outcomes and mortality by sex. Survey-weighted logistic regression analysis was run to identify rates of in-hospital mortality. Linear regression was used to identify trends in length-of-stay.
Results/Discussion: Survivors were younger (mean 62.7 ± 18.3 y; p < .001) and had shorter stays (8.8 ± 11.3d). Every 10-year increase in age increased odds of in-hospital death by 37% (OR 1.37; 95% CI 1.36–1.37). Black (OR 1.31; 1.30–1.33), Hispanic (OR 1.41; 1.40–1.42), and Native Americans (OR 1.57; 1.41–1.75) patients faced higher mortality. Treatment in urban non-teaching (OR 1.38; 1.35–1.40) and urban teaching hospitals (OR 1.69; 1.66–1.71) conferred higher mortality. Uncomplicated (OR 0.91; 0.90–0.92) and complicated diabetes (OR 0.95; 0.94–0.96) were associated with slightly lower odds of mortality. Female sex shortened stays by 8.4%.
Conclusions: Our results indicated that patients with sepsis from poorer sociodemographic areas, minorities, and the elderly had an increase in unfavorable outcomes, and longer lengths of stay. Conversely females and white patients were shown to have shorter LoS and lower rates of mortality.
