(71-STU) Should Internal Medicine Physicians Reconsider the Lymphatic Examination in Breast Cancer Patients? A Cadaveric Study of Axillary Lymph Node Enlargement.
Friday, October 10, 2025

Sara Kurtovic, MPH
Student
Philadelphia College of Osteopathic Medicine - Georgia
Suwanee, Georgia, United States
Presenter(s)
Introduction/Background: Breast cancer metastasis through the lymphatic system significantly impacts prognosis and treatment strategies. Current diagnostic guidelines emphasize breast palpation over detailed lymphatic examination. This cadaveric study examines axillary lymph node size differences in breast cancer versus non-cancer populations and the results may have a broader implication for lymphatic examination.
Methods: Twenty-nine female cadavers (8 with breast cancer, 21 controls) were dissected to collect axillary lymph nodes from six chains: central, humeral, infraclavicular, parasternal, pectoral, and subscapular. Lymph node area (mm²) was measured, and outliers (z ≥ 3) were excluded. Welch’s t-test was used to compare overall node size between groups. A two-factor ANOVA assessed the effects of group, location, and their interaction on node size. Statistical significance was set at α = 0.05.
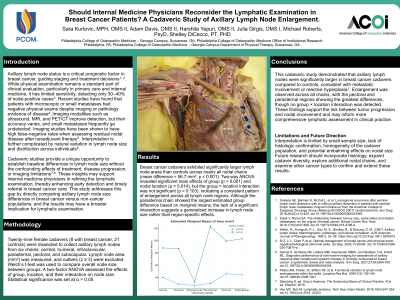
Results/Discussion: Lymph node area was significantly greater in the breast cancer group compared to controls (mean difference = 56.7 mm², p < 0.001). All node chains demonstrated significant group-level differences. The two-factor ANOVA revealed significant main effects of group (p < 0.001) and location (p = 0.014), while the group × location interaction was not significant (p = 0.103), suggesting generalized enlargement across all nodal chains.
Conclusions: This study provides cadaveric evidence that lymphatic involvement in breast cancer extends beyond the regions typically assessed during standard physical examinations. These findings suggest that internal medicine physicians may enhance early detection and treatment by adopting a more comprehensive approach to lymphatic assessment, incorporating both thorough physical examination and timely imaging. Applying this broader diagnostic perspective in clinical practice may lead to earlier recognition and more effective management of lymphatic spread in breast cancer.
Methods: Twenty-nine female cadavers (8 with breast cancer, 21 controls) were dissected to collect axillary lymph nodes from six chains: central, humeral, infraclavicular, parasternal, pectoral, and subscapular. Lymph node area (mm²) was measured, and outliers (z ≥ 3) were excluded. Welch’s t-test was used to compare overall node size between groups. A two-factor ANOVA assessed the effects of group, location, and their interaction on node size. Statistical significance was set at α = 0.05.
Results/Discussion: Lymph node area was significantly greater in the breast cancer group compared to controls (mean difference = 56.7 mm², p < 0.001). All node chains demonstrated significant group-level differences. The two-factor ANOVA revealed significant main effects of group (p < 0.001) and location (p = 0.014), while the group × location interaction was not significant (p = 0.103), suggesting generalized enlargement across all nodal chains.
Conclusions: This study provides cadaveric evidence that lymphatic involvement in breast cancer extends beyond the regions typically assessed during standard physical examinations. These findings suggest that internal medicine physicians may enhance early detection and treatment by adopting a more comprehensive approach to lymphatic assessment, incorporating both thorough physical examination and timely imaging. Applying this broader diagnostic perspective in clinical practice may lead to earlier recognition and more effective management of lymphatic spread in breast cancer.
