(34-STU) Stolen Flow Revealed by the Cuff: A Case of Incidentally Diagnosed Subclavian Steal Syndrome
Friday, October 10, 2025
- MT
Meghan Ta, OMS
Osteopathic Medical Student
Nova Southeastern University KPCOM
Coral Springs, Florida, United States
Presenter(s)
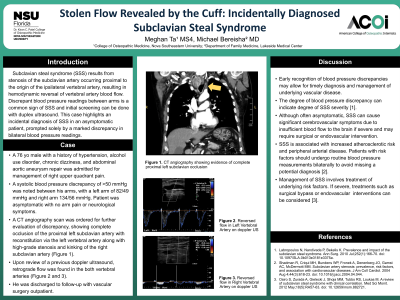
Clinical Scenario or Case: A 76-year-old male with a history of hypertension, alcohol use disorder, chronic gastritis, chronic dizziness, and abdominal aortic aneurysm repair was initially admitted for management of right upper quadrant pain. During a routine vital signs assessment, a significant systolic blood pressure discrepancy of over 50 mmHg was noted between his arms, with a left arm reading of 80/50 mmHg. The patient reported no arm pain or neurological symptoms at the time. A computed tomographic angiography scan was ordered for further evaluation of this discrepancy, revealing a complete occlusion of the proximal left subclavian artery with reconstitution via the left vertebral artery. Upon review of a previous doppler ultrasound, retrograde flow was found in the left vertebral artery and he was subsequently diagnosed with subclavian steal syndrome.
Evidence/Literature Review: Subclavian steal syndrome (SSS) results from stenosis of the subclavian artery that occurs proximal to the origin of the ipsilateral vertebral artery, resulting in hemodynamic reversal of vertebral artery blood flow. While it is often asymptomatic, SSS can cause significant cerebrovascular symptoms due to insufficient blood flow to the brain when severe. Discrepant blood pressure readings between arms is a common sign of SSS and initial screening can be done with duplex ultrasound. SSS can be managed medically with anti-platelet therapy, antihypertensive therapy, and lipid-lowering therapy, but if severe may require surgical or endovascular intervention.
Unique Aspects of Case: This case highlights an incidental diagnosis of SSS in an asymptomatic patient, prompted solely by a marked discrepancy in bilateral blood pressure readings.
Recommendations/Conclusions: Since SSS is associated with increased atherosclerotic risk and peripheral arterial disease, patients with risk factors should undergo routine blood pressure measurements bilaterally to avoid missing a potential diagnosis. Early recognition of discrepancies may allow for timely diagnosis and management of underlying vascular disease.
Evidence/Literature Review: Subclavian steal syndrome (SSS) results from stenosis of the subclavian artery that occurs proximal to the origin of the ipsilateral vertebral artery, resulting in hemodynamic reversal of vertebral artery blood flow. While it is often asymptomatic, SSS can cause significant cerebrovascular symptoms due to insufficient blood flow to the brain when severe. Discrepant blood pressure readings between arms is a common sign of SSS and initial screening can be done with duplex ultrasound. SSS can be managed medically with anti-platelet therapy, antihypertensive therapy, and lipid-lowering therapy, but if severe may require surgical or endovascular intervention.
Unique Aspects of Case: This case highlights an incidental diagnosis of SSS in an asymptomatic patient, prompted solely by a marked discrepancy in bilateral blood pressure readings.
Recommendations/Conclusions: Since SSS is associated with increased atherosclerotic risk and peripheral arterial disease, patients with risk factors should undergo routine blood pressure measurements bilaterally to avoid missing a potential diagnosis. Early recognition of discrepancies may allow for timely diagnosis and management of underlying vascular disease.
