(63-RES) Invasive GAS Pneumonia with Influenza B Co-Infection in Pregnancy: A Case Report
Thursday, October 9, 2025
.jpg)
Thuy Nguyen, DO
Internal Medicine
Jefferson Health Northeast
Philadelphia, Pennsylvania, United States
Presenter(s)
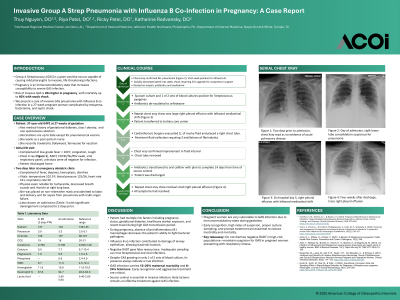
Clinical Scenario or Case: A 37-year-old female at 27-week gestation presented with two days of fever and cough. She worked as an inpatient postpartum nurse and had recently traveled to Dollywood, Tennessee. Work-up including rapid strep test, viral respiratory panel, chest X-ray were negative for infection. She returned two days later febrile, dyspneic, tachypneic, and with hemoptysis. Repeat chest x-ray demonstrated right lower lobe pneumonia, and viral panel confirmed influenza B. She became septic and was admitted to the ICU for norepinephrine infusion. Intravenous empiric antibiotics and oral oseltamivir were started. Within 48 hours, blood cultures and sputum culture grew Streptococcus pyogenes. Antibiotics were de-escalated to IV ceftriaxone. On hospital day 5, repeat chest X-ray revealed new large right pleural effusion with mediastinal shift. Cardiothoracic surgery evacuated one liter of murky fluid from her pleural cavity. She had persistent fluid collection requiring 10 days of chest tube drainage and received three instillations of alteplase and dornase alfa. Antibiotic therapy was transitioned to oral cefdinir to complete a 14-day course from time of source control. She was discharged in good condition one day after chest tube removal.
Evidence/Literature Review: - Hamilton et al., 2013 reports the fatality rate for pregnant women with invasive GAS infections is 15-20% and that increases to 40-60% with progression to septic shock.
- Harris et al., 2023 proposes that pregnancy is an immunomodulatory state that increases the risk and severity of GAS infections.
Unique Aspects of Case: A seemingly benign infection like pharyngitis can lead to severe pneumonia, empyema, and sepsis due to immune system changes during pregnancy
Recommendations/Conclusions: Symptoms of GAS infection can be nonspecific. Clinicians need to have a high index of suspicion even if initial work-up returns negative, especially in immunocompromised populations. Early detection and prompt initiation of antibiotics can prevent progression to invasive diseases and reduce mortality risk for both mother and fetus.
Evidence/Literature Review: - Hamilton et al., 2013 reports the fatality rate for pregnant women with invasive GAS infections is 15-20% and that increases to 40-60% with progression to septic shock.
- Harris et al., 2023 proposes that pregnancy is an immunomodulatory state that increases the risk and severity of GAS infections.
Unique Aspects of Case: A seemingly benign infection like pharyngitis can lead to severe pneumonia, empyema, and sepsis due to immune system changes during pregnancy
Recommendations/Conclusions: Symptoms of GAS infection can be nonspecific. Clinicians need to have a high index of suspicion even if initial work-up returns negative, especially in immunocompromised populations. Early detection and prompt initiation of antibiotics can prevent progression to invasive diseases and reduce mortality risk for both mother and fetus.
